How to Fix Medicaid
The sweeping health-care legislation enacted this spring is many things. It is a vast expansion of federal power. It is a budget-busting entitlement. It is a regulatory nightmare. But to a far greater degree than its advocates have acknowledged, it is also a massive expansion of Medicaid. This means that, under the new law, a hugely expensive program already deep in crisis would not only continue essentially unreformed: It would be put at the very center of America's health-care system.
Medicaid is a joint federal-state program of health coverage for the poor. Its exact rules and practices vary from state to state; generally speaking, however, it is open to people with low incomes (below or just above the federal poverty level) and with some additional compelling condition of need — like being a parent, or having a serious disability. With these eligibility restrictions in place, Medicaid already covers 60 million Americans and accounts for 16 cents of every dollar spent on medical services in the United States.
Under Obamacare, though, people with household incomes up to 133% of the federal poverty level (about $14,400 for individuals, or $29,300 for a family of four) will be eligible for Medicaid regardless of whether they meet any of the other conditions of need. As a result of these loosened eligibility requirements, the bill's proponents expect some 16 million more Americans to sign up for Medicaid between 2014 (when the new rules go into effect) and 2019. This enormous increase in the Medicaid rolls represents about half of Obamacare's projected reduction in the number of uninsured Americans.
On paper, this Medicaid expansion also accounts for about half of the Congressional Budget Office's $940 billion cost projection over the new law's first 10 years. But the effects of expanding Medicaid — one of the most expensive, unwieldy, and perverse creations of American government — will almost certainly be much larger, more extensive, and more dramatic than the CBO's computations suggest.
It is likely, for instance, that far more than 16 million additional people will sign up for Medicaid. As a result of the new eligibility rules, many Americans who are now insured through their employers — but who nonetheless have incomes below the new threshold — will suddenly be eligible for essentially free health care from the government. Many of their employers, as small businesses, will be exempt from any penalties for dropping their employees' coverage. These workers will thus be "crowded out" of private coverage into Medicaid, vastly increasing public costs.
Although there are no hard estimates of the anticipated crowd-out effect of the new law, past experience with Medicaid expansions provides plenty of reasons to be concerned. For example, the National Center for Policy Analysis estimates that of every tax dollar spent on Medicaid expansions during the 1990s, at least half went to new enrollees who dropped their private health plans to join the program, rather than to previously uninsured people. For the related State Children's Health Insurance Program established in the late 1990s, the crowd-out effect averaged about 60%.
Obamacare will therefore put Medicaid increasingly at the heart of our health-care system. For reformers truly interested in "bending the cost curve," this is very bad news: The flaws of the existing Medicaid program — and the extraordinary strain they place on the nation's finances — are high among the reasons why health-care reform is needed in the first place. And Obamacare's exacerbation of those flaws is high among the reasons why the new law will need to be rolled back, and why any serious alternative proposal for improving our health-care system must include Medicaid reform.
THE BOTTOM LAYER
The slapdash way in which a huge and unwieldy expansion of Medicaid became the centerpiece of Obamacare is very much in line with the entitlement's pedigree. From the outset, the story of Medicaid has been one of carelessness, poor planning, and ill-conceived policy design.
The story begins in 1934, when President Franklin Roosevelt appointed a commission to fashion sweeping social-welfare legislation that he intended to champion the following year. The commission's final report proposed the programs that would become Social Security and Aid to Families with Dependent Children, as well as a national health-insurance plan resembling programs that, by then, had already been adopted in several European countries.
But Roosevelt decided that the commission's policy ambitions exceeded his political appetite, and so he left the health-care component out of the 1935 Social Security Act. Still, advocates in and out of government kept pushing. In 1937, another Roosevelt-administration commission outlined a long-term strategy for enacting a "comprehensive National Health Program"; this initiative would have included federal health and disability insurance funded by payroll taxes, as well as federal support for hospitals and federal aid for state medical-assistance programs. Roosevelt did not act on those proposals, but each of them would, in one form or another, become federal law in the course of the following 30 years.
During the 1940s and '50s, a succession of liberal politicians championed national health-insurance legislation only to see their proposals wilt under the glare of unsympathetic voters (and the American Medical Association). So advocates adopted a more incremental strategy. In 1956, Congress and the Eisenhower administration added disability benefits to Social Security. And in 1960, two congressional Democrats — Arkansas representative Wilbur Mills and Oklahoma senator Robert Kerr — teamed up to pitch a federal bailout of failing state programs that provided relief to destitute seniors and people with severe physical or mental disabilities. Unlike calls for universal health care, the Kerr-Mills proposal built on what most lawmakers had long considered to be a legitimate role for government (albeit one that belonged at the state level): to secure housing, sustenance, and basic care for a small group of clearly infirm people whose needs far exceeded their families' resources (and who might otherwise populate street corners or prisons). Mills in particular saw the 1960 legislation as a way to head off any broader, more intrusive federal legislation on health care. He was, of course, mistaken: The program created a precedent for federal bailouts of state relief programs, but without actually appropriating much money for them. Emboldened, hospitals and state governments pushed for more.
In 1964, after resounding Democratic electoral victories, President Lyndon Johnson decided it was time to enact the health-care proposals that had been left out of the Social Security Act nearly 30 years earlier. As the debate began, there were three significant ideas on the table. The main Democratic bill, which reporters soon dubbed "Medi-care," proposed a universal, government-run health plan for senior citizens, to be funded by payroll taxes. A Republican bill that earned the less elegant nickname "Better-care" proposed a voluntary health plan for seniors that would have been funded by a combination of premiums and general tax revenues. A third, bipartisan bill was called "Elder-care" and, unlike previous legislative efforts, had the backing of the American Medical Association; it sought to strengthen the Kerr-Mills system of federal grants to state programs caring for the indigent, the disabled, and poor seniors in nursing homes.
By this time, Wilbur Mills had become chairman of the House Ways and Means Committee, which made him central to the process of crafting the final bill. He decided to take that process behind closed doors and to fashion what came to be called the "three-layer cake" — an amalgam of the three bills. The Democratic bill became Medicare Part A, which provides hospitalization insurance. The Republican bill mutated into Medicare Part B, covering physician charges but retaining only a semblance of voluntary participation and patient premiums. Elder-care morphed into Medicaid — attracting the least legislative attention of the three proposals, and serving primarily to satisfy insistent demands for greater federal support for state health-care programs tending to the poorest of the poor. Compared to the other two components of the legislation, Medicaid was almost an afterthought.
This lack of planning and careful attention certainly revealed itself in the program's haphazard design. Unlike the two parts of Medicare, Medicaid is a joint federal-state undertaking: Each state administers its own Medicaid system, though it must follow broad federal guidelines for the program's design and operation. Funding responsibilities are shared by the federal government and the states in accordance with a formula based largely on the scope of poverty within each state; wealthier states, like Connecticut and Colorado, receive a 50% federal share, while poorer states receive significantly larger federal subsidies. (The largest share this year is Mississippi's, at 74.7%.)
Wilbur Mills and other early champions of the program denied that Medicaid was intended to be another large entitlement; they saw it merely as a safety net for the poorest and most helpless Americans. But it didn't take long for state politicians and lawyers to figure out how to maximize the participation of the able-bodied poor, and for financial advisors to juggle the assets of middle-class seniors so that Medicaid would pay for their nursing-home bills. The sloppiness of the legislation — including the many loopholes it opened up — made out-of-control costs inevitable.
A BALLOONING ENTITLEMENT
The sheer scope of the Medicaid program today would have shocked its designers. Politicians, analysts, and the media tend to focus their attention on the controversial management, rapid growth, and shaky finances of Medicare — and yet Medicaid enrolls more people than Medicare, spends almost as much on hospital and doctor payments, and presents the government and health providers with at least as many fiscal and managerial headaches.
Medicaid is also projected to grow more rapidly than Medicare — and was even before the passage of Obamacare. In fact, if it hadn't been for the Bush administration's Medicare expansion in 2003, Medicaid would probably already be the country's most expensive health-care entitlement. According to the Department of Health and Human Services, Medicare expenditures will be about $516 billion in 2010, while Medicaid (including the State Children's Health Insurance Program) will cost $436 billion (to be shared by states and the federal Treasury).
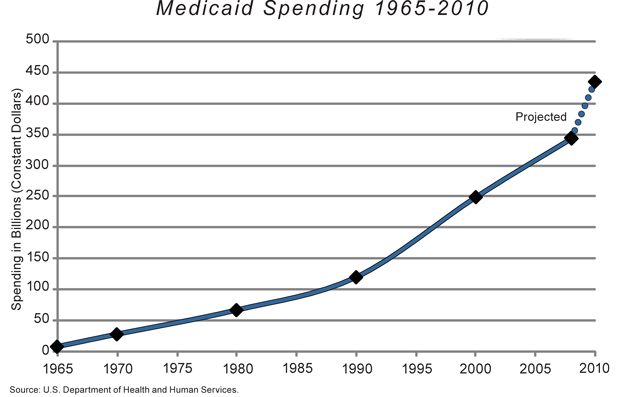
Many factors have contributed to Medicaid's astonishing growth rate. At its inception in 1965, the program cost state and federal taxpayers only $1.3 billion, or about $9 billion in today's dollars. Projected to increase only modestly, annual Medicaid spending (combined state and federal) in fact exploded — to $29 billion in 1970, $68 billion in 1980, $121 billion in 1990, and $250 billion in 2000 (all in 2010 dollars). Obviously, the growth in the cost of health care more generally has outpaced that of most other goods and services during the same period. But in most years since 1965, Medicaid spending has grown faster than either private health spending or Medicare spending.
One reason for this cost explosion has been Medicaid's repeated expansions of eligibility and benefits — expansions that are encouraged by the program's matching-funds design. Under the current system, federal policymakers establish general guidelines, while state policymakers set the specific provisions of their own Medicaid programs. Often, county-level officials are responsible for the actual implementation and enforcement of eligibility and benefit rules.
This shared funding and administration of Medicaid has created a host of perverse incentives, especially for policymakers at the state and local levels. They reap all the political benefits of more generous coverage or looser eligibility rules, but pay only a fraction of the financial cost of such largesse, since the federal government picks up most of the tab. And during downturns and times of lean budgets, state lawmakers will bear the entire political burden if they allow steep eligibility cuts — but will reap only a portion of the fiscal benefits, since most of the cost savings will accrue to the federal government. State and local officials are thus more inclined to spend lavishly on Medicaid than on programs funded entirely by the state.
Moreover, because of both historical accident and the program's design, Medicaid has ended up paying for a very large share of the most expensive of all medical services. From 1960 to 1990, the fastest-growing category of health-care spending was long-term care: stays in nursing homes and home-health visits for elderly and disabled patients. Since 1990, increases in nursing-home spending have moderated some, but the cost of home-based health care has skyrocketed.
Nearly all Americans over the age of 65 are enrolled in Medicare to cover routine doctor visits, hospitalizations, drugs, and other medical services. But Medicare does not cover long-term care or nursing-home stays. For seniors with low incomes, though, Medicaid does pay for such costs: Indeed, it is the single largest payer of nursing-home bills in America (covering 43% of all costs). It also pays one-third of all home-based health-care bills — a number that is projected to grow to one-half by the end of the decade. Thus, as America's population has aged, Medicaid has bloated.
Finally, because Medicaid is, in principle, a means-tested program of public assistance, its design makes it extremely difficult to introduce cost-saving incentives that motivate recipients to think and act like consumers. Federal laws and policies restrict how much cost-sharing states can impose on recipients. And while some states have conducted promising experiments with financial incentives — such as cash accounts managed by recipients — any state's room to maneuver is limited by federal law. Medicaid has also been plagued for years by fraudulent enrollments and claims; such abuse is exacerbated by the fact that the program involves a class of claimants who have little incentive to cooperate with efforts to streamline medical care or reduce long-term expenses.
In short, Medicaid's inherent flaws guarantee that the program's burgeoning costs will endanger America's fiscal health. Like Medicare and Social Security, Medicaid represents an implicit promise of expensive benefits, the costs of which will far exceed future revenues. But unlike the costs of Medicare and Social Security, future Medicaid expenses won't just show up on the books of a heavily indebted federal Treasury: They also represent one of the largest fiscal obligations of state governments, which, for the most part, are not allowed to issue debt for operating expenses. With the program already accounting for more than one-fifth of total state operating budgets, Medicaid growth will mean painful state tax increases, reductions in basic state services like public safety and education, or some combination of both.
Consider the case of California, one of the nation's hardest-hit states. Already facing a $20 billion budget hole in the current fiscal year, California will see its Medicaid caseload rise by nearly 25% after Obamacare is fully implemented in 2014, costing state taxpayers another $2 to $3 billion a year. "We face enormous challenges just sustaining our existing program," California's Medicaid administrator told Bloomberg News in March. "I just don't see states having the capacity to move forward on these changes in this environment."
It is also important to remember that Medicaid is not just a health-care program. It is the largest single component of America's welfare state, far outweighing the dollar value of cash assistance, food stamps, or housing aid. Like these other programs, Medicaid often provides implicit disincentives to work, since increases in income can mean the loss of eligibility for a very valuable benefit. Unless future policymakers introduce reforms to help break the generational cycle of dependency — fixes based on principles that have worked in other welfare overhauls, like time limits and work requirements — the prospect of losing thousands of dollars a year in essentially free health care will perpetuate strong incentives against moving up the economic ladder. Refusing work, or accepting off-the-books jobs with few long-term prospects, will become rational choices for families facing the steep effective tax rates created by the eligibility rules for Medicaid (and soon to be made worse by Obamacare).
In this sense, as in so many others, the new health-care law makes a longstanding problem all the more difficult to solve. But simply rolling back Obamacare's expansion of Medicaid will not be enough: Any genuine reform of our health-care system will need to address the structural flaws that have long been the basis of Medicaid's woes. Doing so will be enormously difficult — as the problem encompasses more than just issues of design, administration, or health economics.
THE MANY MEDICAIDS
While Medicaid does formally exist as a single health-care program administered and financed jointly by states and the federal government, it can also be thought of as an amalgam of four different programs — each with its own caseload, rules, and dynamics.
First, Medicaid is a program for healthy low-income children and some working-age adults. Prior to Obamacare, simply having an income near (or even below) the poverty line would not in itself make someone eligible for Medicaid. Generally speaking, children had to be involved — a rule left over from the era in which welfare was aimed at families lacking a breadwinner. Pregnant women, babies, grade-schoolers, and their mothers have thus made up the majority of enrollees in this category, with some states more willing than others to go beyond these mandatory populations. If Obamacare is fully implemented, this category will grow substantially in the coming years; even now, it represents the largest bloc of Medicaid recipients, accounting for nearly three-quarters of the program's caseload. But it is also the least costly per person: Children and young adults have low average medical claims. About a third of the Medicaid budget is spent on these enrollees.
Second, Medicaid covers individuals with severe physical disabilities. Usually qualifying as a result of their eligibility for the Supplemental Security Income program under Social Security, individuals with significant work-impairing disabilities have traditionally made up a small share of Medicaid recipients. They have, however, consumed by far the most expensive services — which include not just medical care, but often a variety of other benefits, including caregiver assistance with daily tasks as well as room and board.
Third, Medicaid covers individuals with severe mental illnesses or addictions. While technically the two groups of disabled recipients are in the same boat when it comes to eligibility rules — together making up about one-fifth of the Medicaid population, but consuming well over 40% of its budget — it is important to recognize that those suffering from mental illness or substance abuse pose special problems for eligibility determination, case management, and even public willingness to support long-term assistance.
Finally, as discussed above, Medicaid also covers seniors requiring long-term care, and therefore plays a significant role in the lives of many seniors when accidents, diseases, or the inevitable infirmities of age render them unable to perform basic tasks. Those who meet the income test, or can show that their resources will swiftly be spent down to the income threshold, can qualify for Medicaid assistance for institutional or home-based care.
This coverage is intended to ensure that truly poor and ill seniors will not be forced to suffer without the long-term care they need to survive, simply because they cannot pay. The unfortunate reality, however, is that there is now a large industry of lawyers, accountants, and financial planners skilled at arranging the assets of middle-class families so that, when the time comes, their parents or grandparents will qualify for Medicaid. By moving assets around, transferring money or property to children, and otherwise gaming the system, middle-class seniors can save their families the immense cost of long-term care (at the public's expense, of course). In total, seniors account for 10% of Medicaid enrollees — and one-quarter of Medicaid spending.
A great deal of the problem with Medicaid, then, is that unlike with Medicare — which, for all its manifest woes, is a relatively straightforward program — just reaching an agreement about what needs to be fixed (let alone how) is a serious challenge.
For example, recognizing that Medicaid services are the most valuable of the welfare benefits available to low-income Americans, a reform-minded policymaker might want to apply to Medicaid some of the time limits and work requirements that have proven successful in reducing cash-welfare rolls. Such an approach, however, would make little sense in the case of an institutionalized person with a permanent disability. Similarly, measures to encourage families to save, buy insurance, or otherwise prepare for the possibility that aging relatives will need long-term care may help moderate Medicaid's costs in the future. But they won't do much to reduce Medicaid rolls in the short run, given, for instance, the number of seniors already receiving long-term care on the public's dime.
So before we outline a coherent, realistic strategy for reforming Medicaid, we must think through how the various Medicaids we currently have match up with America's financial realities, constitutional principles, and public expectations. After all, what we choose to do about Medicaid depends on how we choose to define federalism, and how we conceive of the proper role of government in providing a medical safety net for a diverse group of citizens — including poor children, the mentally ill, addicts, the disabled, and chronically ill elderly people who have little support from their families or communities.
It is also crucial to think through the difficult political obstacles standing in the way of serious reform — obstacles that have been made all the more daunting by the passage of Obamacare this spring. If Republicans win control of one or even both chambers of Congress in November, they may well be able to revise or, through the appropriations process, slow the implementation of parts of the legislation over the following two years. But an outright repeal of the bill — including the forthcoming Medicaid expansion — would be unlikely to overcome a presidential veto; a complete rollback, therefore, would need to wait until after 2012.
A detailed and forceful case for a different approach, however, cannot wait that long. A clear explanation of Medicaid's problems, of the reasons why expanding the program and putting it at the center of our health-care system would be a disaster, and of the ways in which the program can be improved must be part of the larger case for undoing Obamacare (and for replacing it with genuine health-care reform).
Starting now, reformers need to outline a strategy for fixing Medicaid that conforms with political realities; offers a clear vision of what government should and should not do to subsidize medical assistance; and restores the important roles of individual thrift, family care, private charity, community action, and state policymaking — values that an increasingly federalized Medicaid system has weakened or supplanted.
FIXING MEDICAID
A meaningful reform of the Medicaid system will need to reduce the program's size, scope, and cost to taxpayers; increase self-reliance among the middle class; eliminate disincentives for poor Americans to become middle-class Americans; return power and responsibility to states, localities, charities, and families; and ensure that our scarce public resources actually end up serving those most in need of public help. Policymakers can begin by dividing the work into four key reform elements.
First, they should work to convert Medicaid itself into a more specialized program of medical assistance to those with chronic physical or mental infirmities who are, for all practical purposes, wards of the state. This was, after all, the original idea behind the state-based relief programs that Medicaid was created to bail out nearly half a century ago. Both conceptually and practically, it makes sense to distinguish individuals with chronic medical conditions — those likely to produce long-term dependency on the state — from healthy individuals who, due to job loss or other short-term emergencies, find themselves without health insurance or savings. Medicaid ought to be focused on the needs of the former, not the latter; efforts to provide a temporary safety net to people who are, by and large, working and contributing members of society should take a different form. Congress should rewrite eligibility standards accordingly, creating a separate program to subsidize private health-insurance premiums for the able-bodied poor (as described below).
As for the management of the remaining long-term Medicaid caseload, states should receive more latitude to experiment with initiatives to coordinate care, both within the practice of medicine and between Medicaid and other state agencies. For example, state agencies need to work together to avoid creating massive costs for one another — such as when a Medicaid-eligible patient with severe mental illness or addiction goes off his medications, commits crimes or public disturbances, ends up in jail, and then gets transported to a psychiatric hospital or detox center. Tracking patients through the system can help limit these destructive cycles.
In experimenting with such initiatives, states should be careful to avoid the myth of prevention savings: the notion that spending more money on the front end can save much more money on the back end. Preventive medicine is often good medicine, as it helps avoid chronic diseases like diabetes or heart disease; but, as decades of data have shown, it does not save money. Preventive medicine is itself quite expensive, and in most cases people who consume a preventive service would not have needed a more expensive intervention later on anyway (that is, they would not have developed diabetes or heart disease even without the preventive care). As a result, the costs to the system as a whole outweigh the financial benefits. Preventive care must therefore be counted as an expense — even if often a worthwhile one — not a savings.
There are, of course, other proven and effective ways to save — by using vouchers to encourage careful spending or by assigning case managers to help recipients use their benefits efficiently, for instance. And while there is no silver bullet, state policymakers should be encouraged to try those streamlining efforts that they think stand the best chance of reducing Medicaid waste in their states. Above all, states must have the right incentives to lower costs — for example, the ability to keep all of the potential savings from a politically difficult yet effective reform — as well as good reasons to strictly enforce eligibility rules, so that new costs do not overwhelm any savings their reforms might produce.
Second, policymakers should convert Medicaid coverage for low-income but healthy children and working-age adults into a system that subsidizes the payment of premiums for private health-insurance plans. For instance, a future Congress could convert Obamacare's bewildering array of cash payments and tax credits into a universal tax credit, conferring what amounts to an exemption from income and payroll taxes for a fixed amount of household spending on (or saving for) health care.
The tax credit could take the place of the existing unlimited exemption for employer-based plans (as proposed by John McCain in his 2008 presidential campaign, and by several Republican members of Congress since). Such a fixed-dollar credit would be worth most to individuals with children and low incomes, reversing the current dynamic in which unlimited tax deductibility confers the greatest benefit on upper-income Americans and those who work for large employers. Families would be free to apply their tax credits to the purchase of health plans and toward health savings accounts (into which states should be allowed to contribute additional funds now earmarked for Medicaid to help lower-income people).
The key to a successful system of direct premium supports for jobless or low-income Americans and their families, however, is ensuring that it is thought of more as a welfare program than as a health-care program. Recipients should be required to meet the same work or job-search rules currently required for cash welfare benefits. The intention should be to provide temporary, transitional assistance for those down on their luck, not a means of perpetuating dependency.
Third, policymakers should convert the current complex system of federal Medicaid funding into annual block grants to the states, adjusted annually to accommodate medical inflation. Today, Medicaid is an open-ended entitlement: The states set eligibility standards, spend money to cover services for people who meet those standards, and essentially bill the federal government for its share of the costs on a rolling basis. The levels of spending are therefore never fixed, and states do their best to extract more money from Washington by gaming the system's arcane rules.
A single annual block grant would instead allow state policymakers to know exactly how much federal money they will receive for the year and to budget accordingly; it would also allow federal policymakers to have more predictable levels of spending. An added benefit of a block-grant system is that it would give state governments more responsibility for their Medicaid funding: If states choose to expand eligibility or benefits in their programs, they should be required to raise the additional funds beyond their block grants (either by cutting spending elsewhere, or raising taxes). Because most states must balance their budgets every year, they won't be able to paper over Medicaid expansions with additional debt, as Washington can do. Forcing states to responsibly manage one lump sum of money will thus make it harder for government to deceive taxpayers about the real costs of the program. And on the other side of the ledger, states should be able to recoup most of the savings from any disease-management initiatives, asset-recovery programs, or benefit reductions they implement, rather than being forced to send most of the savings they may obtain (often at great effort and political risk) back to Washington to be redistributed to other, more profligate states.
As for Medicaid's current array of mandatory and optional services, federal policymakers should simplify the rules by setting the initial federal grant at the amount required to fund only mandatory services (like doctor visits and hospital stays). States would be allowed to provide additional coverage (for medical needs like dentures and eyeglasses), but only using their own dollars.
This would be a marked departure from the current system, under which state politicians have generally been able to expand Medicaid services and eligibility only to the extent that they could convince voters that the increases would be funded largely by the federal government. Some politicians have been more successful at selling this argument than others, which is why there are such enormous differences in Medicaid spending across the states. Moreover, while liberal states typically offer more generous programs and politically conservative states offer less generous ones, there does not seem to be much evidence that the states with more generous Medicaid programs have better health outcomes. So by getting the federal government out of the matching-grants business — and by letting states make and fund their own decisions about program expansions — policymakers will increase the likelihood that any additional tax dollars committed to Medicaid will make a real difference in the quality and availability of medical care.
Of course, one big political obstacle to block granting will be the debate over setting the initial grant baseline. Higher-spending states will want to freeze their current funding levels in place, which lower-spending states will see as unfair. Although a block-grant conversion would confer fiscal benefits on the country regardless of the starting point (by encouraging wiser spending decisions in the states), it would be preferable for Washington to set a baseline that, as much as possible, allocates a similar amount of federal funding per mandatory enrollee, adjusted for regional differences in medical prices. Under such a computation, New York would still receive substantially more federal dollars per low-income person than Mississippi; the difference in actual purchasing power, however, would be minimal.
Fourth, policymakers should encourage American families to save for long-term care. Beyond reversing Obamacare's attack on tax-free health savings accounts, this can be achieved by establishing generous tax relief for private long-term-care insurance, by dramatically tightening Medicaid eligibility rules, and by seriously stepping up eligibility enforcement.
While statistics show that most Americans entering retirement will not require lengthy and expensive nursing-home stays, some certainly will. Even more seniors face the prospect of other long-term expenses, such as home-based health care. Furthermore, the share of the population over the age of 85 is expected to increase by more than 50% in the next 15 years (as older people are in better health than ever before), so we can expect a significant increase in the number of seniors needing long-term care.
As with other major life expenses — like sending a child to college, or losing a job — public policy should encourage families to plan for the possibility of long-term care through prudent saving and insurance coverage (rather than encouraging reliance on the government to pay the bills, using taxes collected from thriftier families). And one obvious way federal and state policymakers can encourage thrift is by changing tax policy — restoring, and expanding, the health savings accounts that Obamacare strictly limits, and creating the aforementioned universal tax credit for health care (including the purchase of long-term-care insurance).
Still, those who study and sell such insurance insist that tax incentives alone won't be enough to induce American families to take the necessary steps to protect their assets against future long-term health-care expenses. The Medicaid-fraud industry of lawyers, accountants, and benefits consultants has been too successful in marketing the message that, with creative planning, middle-income families can ensure that their elderly relatives will qualify for Medicaid.
The only realistic way to change this public perception is to change the law so that it becomes both difficult and unappealing for middle-class seniors to qualify for Medicaid. To begin with, it should be made more difficult for people with expensive homes to receive coverage. Today, an individual's home equity up to $500,000 (and in some states up to $750,000) is excluded from the calculation of assets when determining Medicaid eligibility. Congress should set a date — far enough into the future to reduce political blowback and to allow families to adjust their plans — for phasing out all exemptions of home equity from these calculations. In addition, the existing rules against seniors' transferring assets to family members in order to meet Medicaid eligibility requirements — which take into account transfers of wealth reaching back five years before a person applies for Medicaid, and then limit that person's eligibility based on the amount transferred — should be extended to reach back at least 10 years.
At the same time, states should be far more aggressive in enforcing these rules, keeping in mind that every dollar not spent subsidizing the inheritance of a middle-class family is a dollar that can be spent on a truly needy senior with no family to rely on. Americans should be made to understand that if they want to place a relative in long-term care through Medicaid, they will have to either spend down all of the relative's assets — including the value of a home — or transfer those assets to the state after the relative's death (as current law already requires when a senior turns out to have had more assets at the time of his death than when he applied for Medicaid coverage). Families must be made to recognize that if they want to avoid these unpleasant eventualities, they will need to buy private insurance — not try to game the state.
STEPPING BACK FROM THE ABYSS
Reforming Medicaid has never been an easy prospect — and the passage of Obamacare has only made it more difficult. Many of the most powerful lobbies in Washington and in state capitals will work against any effort to fix what ails this deeply flawed entitlement. Liberal politicians, too, will obstruct the reform process at every step, recognizing (correctly) that such a restructuring of Medicaid would move America as far away from their ultimate goal — single-payer, government-run health care — as Obamacare moved America toward it.
But the simple truth is that American taxpayers cannot afford the status quo. Even before Obamacare, the combined cost of Medicaid, Medicare, and Social Security was projected to consume nearly 15% of gross domestic product by 2030 — up from less than 10% today. These entitlements are already falling into the red, and have an unfunded liability of nearly $100 trillion through the end of the century.
Obviously, all three programs are in need of serious change. But from the perspective of America's long-term fiscal health, Medicaid presents the most urgent challenge — because the program involves state governments that have far fewer options for contending with debt than Washington.
As much as Obamacare has complicated matters, it has also stirred up a great deal of public furor. This presents policymakers with an opportunity to roll back the law, and to implement meaningful reform of Medicaid in its place. Given what is at stake for the nation, it is an opportunity Americans cannot afford to let pass by.